This guide explains what patients typically do, what they can expect, and how to get the most accurate result.
What is a home sleep study, and who is it for?
A home sleep study Adelaide service involves an overnight test that records breathing, oxygen levels, heart rate, and sleep-related airflow patterns. It is most commonly used to investigate suspected obstructive sleep apnoea and snoring-related breathing issues.
It often suits people with straightforward symptoms such as loud snoring, witnessed pauses in breathing, morning headaches, or daytime sleepiness.
How do patients in Adelaide usually get a home sleep study organised?
They usually start with a GP, sleep physician, dentist with a sleep focus, or a sleep clinic referral pathway. The clinician reviews symptoms, medical history, and risk factors, then decides whether a home test is appropriate.
If a home study is not suitable, they may be directed to an in-lab polysomnogram instead.
What happens before the night of the test?
They receive a device kit and instructions, either by pickup, delivery, or in-clinic fitting. Most services explain how to place each sensor, how to start the recorder, and what to do if something comes loose overnight.
Patients should confirm the return method and timing, and ask who to contact after hours if there is a device issue.
How do they set up the device at home?
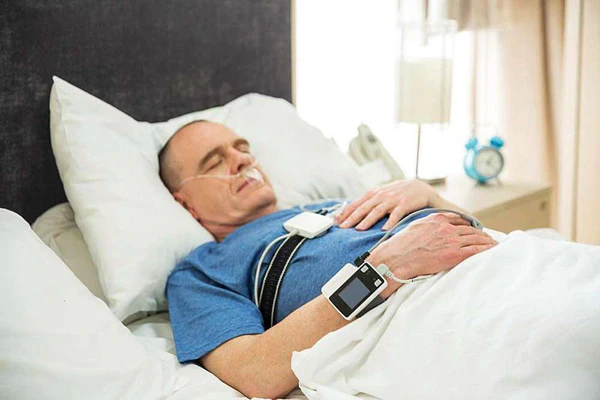
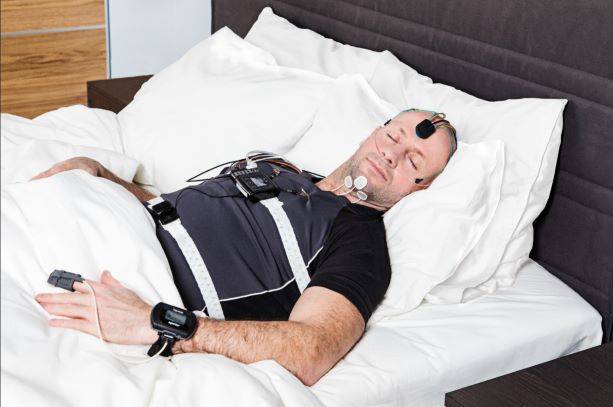
They follow the provided steps and fit the sensors snugly before bed. Most home sleep studies use a combination of a finger probe (oxygen), chest or abdomen belt (breathing effort), and a nasal cannula (airflow), plus the main recorder.
They should keep the setup as close as possible to the instructions, because poor sensor contact can affect data quality.
What should they do on the day and night to improve accuracy?
They should aim for a typical day and a normal bedtime routine so the study reflects real sleep. Unless their clinician says otherwise, they should avoid heavy alcohol intake and sedatives, since these can change breathing patterns and worsen snoring and apnoea.
They should charge the device if required, keep pets away from tubing, and secure cables to reduce the chance of dislodgement.
What if they wake up and something has come off?
They should reattach it as soon as they notice, using the instructions in the kit. If the device has indicator lights or an app, they can check whether recording is still active.
If they cannot restore the setup, they should continue sleeping and report the issue when returning the equipment, since partial data may still be useful.
What happens after the test night?
They return the equipment as directed, usually the next business day. The provider downloads and checks the recording, then a clinician interprets the results.
If the data is incomplete, they may be asked to repeat the study, particularly if key sensors were off for long periods.
How long does it take to get results, and what do they usually include?
Results timing varies, but many services provide a report within several days to a couple of weeks. Reports commonly include an apnoea-hypopnoea index (AHI) or respiratory event index (REI), oxygen desaturation information, and snoring or airflow disturbance patterns.

They should ask for a clear explanation of severity and what it means for symptoms and long-term health.
What are the most common next steps if the study suggests sleep apnoea?
They may be offered CPAP therapy, a mandibular advancement splint (for suitable cases), positional therapy, weight management support, or further specialist review. The best option depends on severity, anatomy, comfort preferences, and other health conditions.
If symptoms are strong but the home study is negative, they may be referred for an in-lab study to rule out other sleep disorders.
When might a home sleep study not be enough?
It may be less suitable for people with significant heart or lung disease, suspected central sleep apnoea, complex insomnia, parasomnias, or suspected narcolepsy. In those cases, an in-lab study can measure more signals, including brain activity, which helps stage sleep and detect a wider range of disorders.
They should rely on clinician guidance rather than self-selecting a test type.
What should patients ask the provider before booking in Adelaide?
They should ask whether the service includes clinician interpretation, follow-up, and treatment pathways. It also helps to confirm total costs, any Medicare or private health rebate options, and what happens if a repeat night is needed due to poor data.
They should also ask who receives the report, such as their GP, a sleep physician, or both.
FAQs (Frequently Asked Questions)
What is a home sleep study and who is it suitable for?
A home sleep study is an overnight test conducted in your own bed that records breathing, oxygen levels, heart rate, and airflow patterns to assess suspected obstructive sleep apnoea and snoring-related issues. It is ideal for individuals with straightforward symptoms like loud snoring, witnessed breathing pauses, morning headaches, or daytime sleepiness.
How do I arrange a home sleep study in Adelaide?
You can start by consulting your GP, a sleep physician, a dentist specializing in sleep disorders, or through a sleep clinic referral pathway. The clinician will review your symptoms and medical history to determine if a home sleep study is appropriate or if an in-lab polysomnogram is needed instead.
What should I expect before and during the night of my home sleep study?
Before the test night, you’ll receive a device kit with instructions on sensor placement and device operation. On the night of the study, you should set up the sensors snugly as instructed—commonly including a finger probe for oxygen levels, chest or abdomen belts for breathing effort, and a nasal cannula for airflow—and follow your normal bedtime routine to ensure accurate results.
How can I ensure accurate results during my home sleep study?
Maintain your typical daily activities and bedtime routine while avoiding heavy alcohol and sedatives unless advised otherwise by your clinician. Make sure the device is fully charged if required, keep pets away from tubing, secure cables to prevent dislodgement, and promptly reattach any sensors that come loose during the night following the provided instructions.
What happens after completing my home sleep study?
After returning the equipment as directed—usually the next business day—the provider downloads and reviews the data. A clinician interprets the results which typically include indices like the apnoea-hypopnoea index (AHI), oxygen desaturation levels, and snoring patterns. If data quality is poor or incomplete, you may be asked to repeat the study.
What are common treatment options if my home sleep study indicates sleep apnoea?
Treatment may include CPAP therapy, mandibular advancement splints for suitable cases, positional therapy, weight management support, or further specialist evaluation. The best approach depends on factors such as severity of apnoea, anatomy, comfort preferences, and other health conditions. Negative results with persistent symptoms might warrant an in-lab study for further investigation.